by Adam D Barlow, Department of Surgery, University of Cambridge
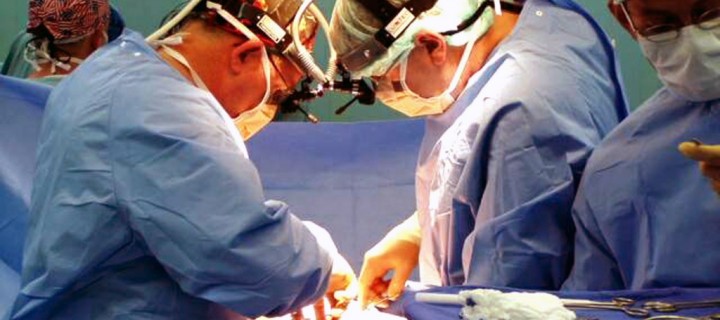
Solid organ transplantation provides life-saving treatment for infants and children with liver and cardiac failure, and is the best treatment for end-stage renal disease. In the UK in 2012/2013, 25 infants (<1 year of age) received organ transplants comprising four heart, 17 deceased donor liver and four living donor liver transplants, and as of January 2014, five infants were on the liver transplant waiting list and three were awaiting a heart transplant (personal communication with National Health Service Blood and Transplant (NHSBT)). While infants form only a very small minority on the active transplant waiting list, they are at a significantly higher risk of mortality, with 31% of infants on the cardiac transplant waiting list dying before receiving a transplant. Furthermore, infants have the highest mortality of all patients on the liver transplant waiting list. The principle reason for this excess mortality is a lack of suitable infant donors. Given that over a third of all paediatric deaths in the UK occur in the neonatal period, expanding organ donation in the neonatal population would address this imbalance as well as improving the supply of organs for older children on the transplant waiting list. Currently in the UK, organ donation is not permitted from brain-dead infants <2 months of age. This is due to the current guidance on the diagnosis of brainstem death (BSD) which states that it is rarely possible to confidently diagnose BSD in infants between 37 weeks’ gestation and 2 months of age, and that before 37 weeks’ gestation, the diagnosis of BSD is inappropriate. However, this guidance has not been updated since 1991 and is at odds with current practice in other countries such as USA, Australia, Canada and many European countries, who accept the concept.